Without a firm belief in the benefit of the innovation for patients, they won’t succeed. A conversation with three such innovators who, thanks to their patience and tenacity, have succeeded in making maternity care more patient-friendly.
Martine Kerkhof and Marco van Elst are daughter and son-in-law of Chris Kerkhof, the man who brought Sense4Baby to the Netherlands. Sense4Baby is a mobile device that can be used at any desired location for foetal heart rate monitoring, known as CTG. Chris worked at a company that sold a predecessor to this product. In the Netherlands, it failed to get a foothold in the market due to the dominant position of Philips in the hospitals. Therefore, in 2007 he came up with a new business model: to have CTGs performed outside the hospital, in the pregnant woman’s own home by a specially trained nurse.
He found that several hospitals were open to this innovative form of telemonitoring. ‘At that time, the home monitoring of patients didn’t exist at all. My father really was the first one,’ says Martine Kerkhof. Where during the Covid pandemic hospitals had to discharge patients early and monitor them at home out of pure necessity, because there simply wasn’t enough space in the hospital, Sense4Baby was developed in the interest of the expectant mother and her unborn child. After all, it’s stressful enough if there are problems with the pregnancy. If on top of that you also have to go to the hospital, sometimes daily, to have a CTG carried out for 40 minutes, that doesn’t exactly help reduce the stress.
Success, but no customers
And so, the first virtual hospital in the Netherlands was established: Stichting Telenatal, set up as an independent treatment centre. Telenatal had contact with the pregnant women, instructed the nurses on how to fit the CTG and read out the CTG data remotely. The results were shared with the hospital obstetricians, whose workload was considerably reduced. Kerkhof quickly found other hospitals that were willing to work together in this way. Together they showed that the costs of maternity care decreased through the home monitoring of pregnant women. What’s more, the quality of care increased. And patient satisfaction was extremely high.
In the last few years the market has started to change. eHealth and telemonitoring are firmly on the rise, also in other medical specialties.

‘Despite the good results and the enthusiasm of the participating hospitals, patients and health insurance providers, only very few additional customers could be found,’ says Marco van Elst, who has worked for the company founded by his father-in-law since 2012 and who became shareholder and CEO in 2013. ‘Chris first set up the virtual hospital for the company he worked for then. That company was taken over and the new parent company didn’t want to take it forward. So my father-in-law decided to continue on his own via a management buy-out. He asked me to join the business.’
Marco’s sister-in-law Martine Kerkhof, Chris’s daughter, also went to work at Telenatal. ‘I have a background in medical technology and already worked in sales in medical equipment when my father started out on his own and needed some help. He’d discovered that, as a small independent company, it’s extremely difficult to enter the healthcare market. Having a big name behind you is at least as important as the quality of your product. This was highlighted all the more by the presence of a single dominant player in this market, which didn’t have any telemonitoring solution itself. Large players can develop a market, but for a small start-up that’s far more difficult,’ says Martine.
Start-ups have to rely on their inventiveness and their ability to align far more closely with developments in the market. In this way, new applications for the product quickly emerged, such as having CTGs performed by primary-care midwives. Maternity care in the Netherlands is characterised by the independent primary-care midwifery practices that monitor pregnant women with uncomplicated pregnancies and deliveries. This may be at the client’s home, or as an outpatient in the hospital. Despite these new developments, things still weren’t great for the start-up financially, or for its founder. Chris got sick. In 2017, three months after Martine gave birth to a healthy baby boy, he passed away. ‘That was an extremely difficult period for our whole family. I was being tossed around by all kinds of emotions and couldn’t be of value to the company. Fortunately, Marco didn’t give up and saw the situation as an impetus to fight even harder,’ says Martine.
Definitive breakthrough
That battle resulted in Van Elst finding a new shareholder who believed in the product just as much as he did: ICT Healthcare Technology Solutions (HCTS). With new energy, room for investment and extra people they finally succeeded in expanding the market. Because in the meantime a variety of services had become available, the physical product was given a new name: Sense4Baby. Now, hospitals in eight European countries use this technology to monitor pregnant women at home. In addition, in various regions in the Netherlands, it is used to carry out CTGs by primary-care midwives.
Van Elst: ‘In the last few years the market has started to change. eHealth and telemonitoring are firmly on the rise, also in other medical specialties. Government-initiated programmes such as “De Juiste Zorg op de Juiste Plek” (The Right Care in the Right Place) have led all hospitals to consider which care provision they can shift from the secondary to the primary setting or to the patient at home. As a result, hospitals now see things differently than they did a few years ago, although often there’s still a lot of convincing to be done.’
During the Covid pandemic, ICT HCTS made Sense4Baby freely available to hospitals without obligation; after all, in the spring of 2020, hospitals wanted to minimise the number of patients visiting the hospital. ‘It was wonderful to be able to make a contribution in such an emergency situation, no matter how small,’ says Van Elst.
Also in primary care
As already mentioned, midwifery practices have also started to perform and interpret CTGs. This is something that was never done in the past, even though midwives are taught how to interpret CTGs during their training. It’s thanks to midwife Siegrid Hoekstra that all insurance providers have embraced the idea and that the Dutch Healthcare Authority has decided that a nationwide rate will be introduced from 2023.
It’s no coincidence that Hoekstra has been the driving force behind CTGs in primary care, given that she was also instrumental in other innovations such as the 20-week ultrasound scan in the Midwifery Centre Nijmegen and the turning of breech babies by the midwife instead of a hospital obstetrician.
During a study trip to Canada in 2012, she saw how routine it was for midwifery practices to carry out CTGs themselves. ‘Because of the huge distances in a country like Canada, you don’t want to send pregnant women to the hospital for every possible complication.
Take an indication like reduced foetal movement, for instance. Nine out of ten times there’s nothing wrong and the CTG is normal.
But of course it’s very stressful for women if they have to go to the hospital. They’re left worrying for longer than necessary and travelling in the later stages of pregnancy also isn’t much fun. What’s more, as an expectant mother you will already have developed a close bond with your midwife. In the hospital you’ll see a healthcare provider whom you’ve never met before.’
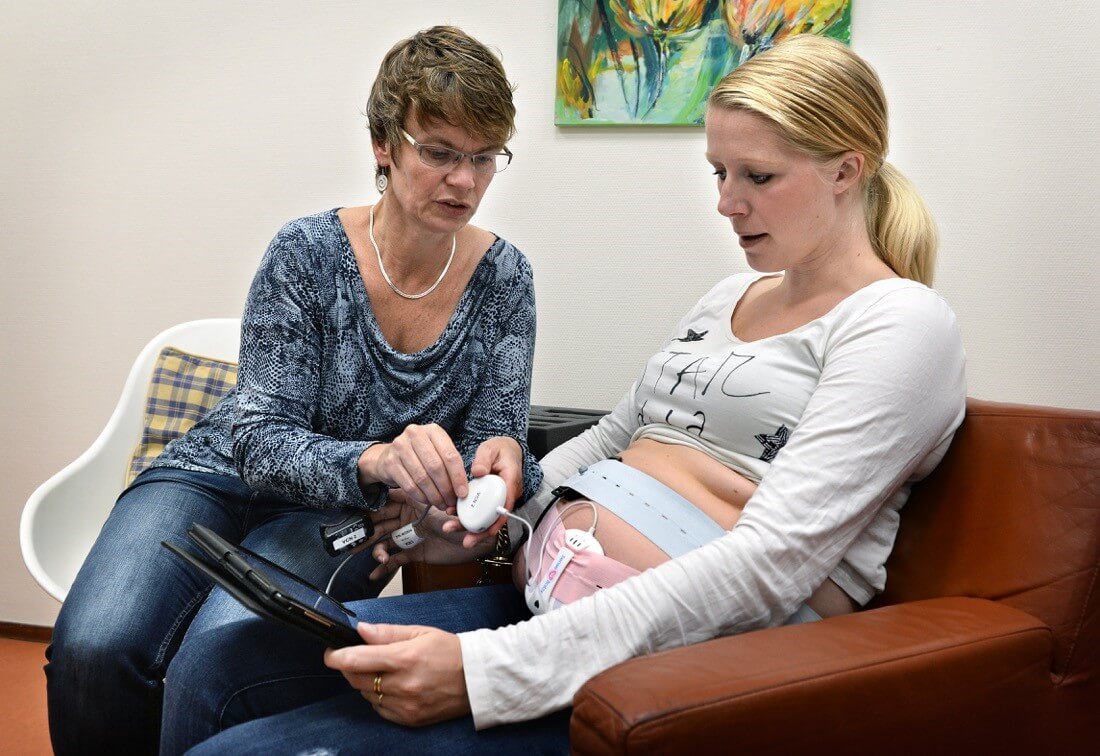
Six-year pilot project
Back in the Netherlands, Hoekstra encouraged other midwives within the cooperation that the Midwifery Centre Nijmegen is involved in to consider: could this kind of model be feasible in the Netherlands?
If so, for which indications could you perform a CTG in the midwifery practice? How often do we see these indications in our region? And how would this impact the midwives’ workload?
She drafted a plan and discussed this with health insurance provider VGZ, a company she knew from previous innovations. VGZ gave the green light to set up a pilot project. Hoekstra: ‘The broad picture was clear, but then you have to work out in detail how you’re going to organise things. Which protocols are we going to use? How do we safeguard quality? What additional training do midwives need to follow to be able to perform a CTG themselves? Which technology are we going to use?’
It took a year to work through all the details. In 2015, 14 midwifery practices and two hospitals in the Nijmegen region started performing antenatal CTGs in the primary care setting for three indications: if a woman notices reduced foetal movement, after a breech baby has been turned, and if a woman is past her ‘due date’ (post-term pregnancy).
Incredible results
We’re now six years and countless CTGs further. The results have been incredible. In 86% of cases it wasn’t necessary to refer the woman to the hospital. That saves a huge amount in healthcare costs. The women gave the care provision an average score of 9.4. And the obstetricians are extremely satisfied. They are actively involved and see that midwives evaluate the CTGs exceptionally well. In case of doubt, obstetricians can view the CTGs remotely.
Janneke Banken-Croonen, director of the Midwifery Centre Nijmegen: ‘By performing CTGs within primary care, we increasingly see the right care provided in the right place, and that the collaboration between midwives and obstetricians has improved. The mobile CTG device enables midwives to provide this care easily and relatively inexpensively. Including a CTG in their consultations also fits within the midwives’ remit. After all, evaluating CTGs is part of the training.’
However logical it is, Banken-Croonen also realises that you need people like Hoekstra, people who are determined and who will defend the interests of their clients whatever it takes. Otherwise, the system doesn’t change.
All in all, we’ll soon be 10 years on from the first idea to have CTGs performed by primary care midwives, and 15 years on from the emergence of the technology. Without the passion and enthusiasm of people like Siegrid and Chris, it would never have succeeded.
Many people would have given up long ago. But they carried on, even when things got difficult. At the start of the project, there were doubts about the quality of the CTG evaluations by the midwives. This made Siegrid work even harder to organise good quality assurance, in order to prove: “we can do this”. Without her passion and energy, the project would’ve floundered long ago.’
Instead, thanks to her commitment and enthusiasm, the regions Amsterdam and Zwolle also recognised the opportunities and joined the project. Since then, the regions Kennemerland, Emmen and Helmond have also introduced CTGs within primary care, although the hospitals and midwifery practices involved organise things slightly differently, outside the project.
Fourteen years from concept to mature market
It’s been 14 years since Chris Kerkhof developed the concept of a virtual hospital and started the remote monitoring of pregnant women; only now is the movement so big that everyone is confident that it won’t be ‘rolled back’. Nowadays, there are simply too many hospitals, midwives, patients and insurance providers who have seen and experienced that things can be set up differently. Martine Kerkhof is emotional when she says: ‘It’s such a shame that my father never got to see this success. He died a year after the pilot project in Nijmegen started, but before large-scale results came in and things really took off. We aren’t there yet: only when every pregnant woman can opt for this solution will we have achieved our goal. But we’ll get there. The thing that my father would’ve been most pleased about, is the score of 9.4 that patients at the Midwifery Centre Nijmegen gave this care. Because that’s where it all started for him: good-quality, safe care for the mother and her unborn child.’
